ARTICLE SUMMARY:
The COVID-19 pandemic has brought telehealth and other remote healthcare technologies into the spotlight. Recent efforts to loosen coverage restrictions and increase availability and adoption of these care options could have a wide-reaching impact on health technology markets that lasts well beyond the current crisis.
Telehealth has emerged as a key tool in the fight against the novel coronavirus, and providers, insurers, government agencies, and telehealth companies are all taking steps to make this important remote healthcare resource more widely available in the US. Clearly, this is a pivotal moment for the US telehealth industry, which has struggled for decades to gain acceptance and momentum. In recent years, reimbursement hurdles have begun to fall, prompting a rise in telehealth adoption; however, the market remains vastly underpenetrated.
Telemedicine’s historically tepid growth trajectory could get a dramatic boost in the weeks and months ahead as remote screening and monitoring is expanded across the nation to help deal with the current pandemic and stakeholders become more aware of its capabilities and benefits. In fact, depending on how smoothly the ramp-up goes over the next several months, it is quite likely that some of the temporary moves recently put in place to enable wider access to telemedicine during the coronavirus crisis—such as those that greatly expand coverage for Medicare patients—may become permanent once the pandemic is over.
But the long-term implications are not limited to the telemedicine industry. As virtual and home-based healthcare (and even remote, digitally enabled clinical trials) become more commonplace, demand will grow for digital diagnostic and monitoring tools and technologies that can enable this shift, and medical device and technology companies well positioned to fill that need will be among the biggest beneficiaries.
Barriers to Medicare Coverage Fall
The telehealth industry has been slowly turning the corner over the past few years, as many large healthcare systems and private insurers took the lead in adopting and promoting telemedicine and remote care as a way to improve the patient experience, potentially reduce costs, and address physician shortages, which are particularly acute in some specialties. As is often the case, this positive momentum was driven in large part by progress on the coverage and reimbursement front—progress that involved not only telemedicine services, but also the growing list of digital remote monitoring technologies now available that enable more comprehensive remote care.
In the case of telemedicine, private payors have been leading the way, but remote monitoring technologies and services have made recent inroads in both the private and public sectors. (See “New Rules and Regs Push Telehealth into the Mainstream,” MedTech Strategist, October 4, 2019 and “Consumerism Drives New Interest in Virtual Care Models, but Challenges Persist,” MedTech Strategist, June 16, 2017).
But by far the biggest recent boost for the telemedicine industry came in mid-March of this year when CMS announced it was easing restrictions on telehealth for Medicare fee-for-service patients, a move taken in response to the COVID-19 epidemic but one that many in the industry say was long overdue. Many private insurers also weighed in, waiving deductibles for telehealth visits in order to aid social distancing efforts and help slow the rapid growth of COVID-19 cases.
Summary of Recent Telemedicine Waivers
Sources: CMS; MedTech Strategist |
The changes from CMS are particularly important for the telehealth industry since they represent a notable policy shift that could have a lasting impact. Historically, Medicare coverage for telehealth has been very limited, although many people enrolled in Medicare Advantage plans and those on Medicaid have had greater access to telehealth services through private insurers and individual states. Prior to these waivers, CMS only covered telehealth services for Medicare fee-for-service (FFS) beneficiaries who lived in designated rural areas, and the telehealth visits had to be conducted in a clinic or other medical facility—remarkably, telehealth conducted in the patient’s home was not covered. The waivers remove all these restrictions—Medicare FFS beneficiaries can now receive telehealth services no matter where they live across the US, and the virtual visit can take place anywhere, including in the patient’s home. Importantly, these telehealth services will be paid under the Physician Fee Schedule at the same amount as in-person services, and even though these changes were enacted during the coronavirus health crisis, the new coverage rules apply to all Medicare beneficiaries, not only those who have, or are suspected to have, COVID-19.
The impact of expanding remote care during this crisis and beyond could be particularly important for patients with chronic conditions. According to CMS, 29% of Medicare FFS beneficiaries have two to three chronic conditions and 15% have six or more. These patients are the costliest to care for and the most at risk during a pandemic. Studies suggest telehealth and other remote care services and technologies may be able to generate cost savings in this population by addressing problems before they become more serious and helping to eliminate barriers to timely care. Overall, there are 100 million Americans with chronic conditions today, according to the American Medical Association (AMA). AMA recently issued a statement praising the moves by CMS and encouraging private payors that are not already covering telehealth services to do so now to ensure “uninterrupted care” for chronically ill people during the COVID-19 pandemic.
In addition to these developments, the $2 trillion economic stimulus package recently signed into US law provides even more support for telehealth. Among other things, it further expands the settings and circumstances under which Medicare will cover telehealth, provides monetary support so that more providers can increase their telehealth capacity (including Indian Health Service and the VA), and instructs HHS to issue clarifying guidance encouraging the use of technologies such as remote patient monitoring during the COVID-19 emergency.
Demand on the Rise
Analysts expect these changes to result in a substantial boost for telehealth companies like Teledoc Health Inc., American Well Corp., and others in the months ahead. Not only do Medicare patients represent a huge, underserved market for telehealth, there is some data suggesting that Medicare beneficiaries, when provided with telehealth, may use the service more frequently than the average commercial user. According to a report issued by CMS in November 2018, only 90,000 out of 35 million Medicare FFS beneficiaries (about 0.25%) utilized telehealth services in 2016, although the data showed significant growth in utilization among the oldest group (those age 85 and older). But the 90,000 users racked up a total of 275,199 telehealth visits during the year, a rate of about three visits per person, which is about two-times the utilization rate reported in the past for commercially insured users. (Of note, in 2016, the most common use for telemedicine among Medicare patients was psychotherapy.)
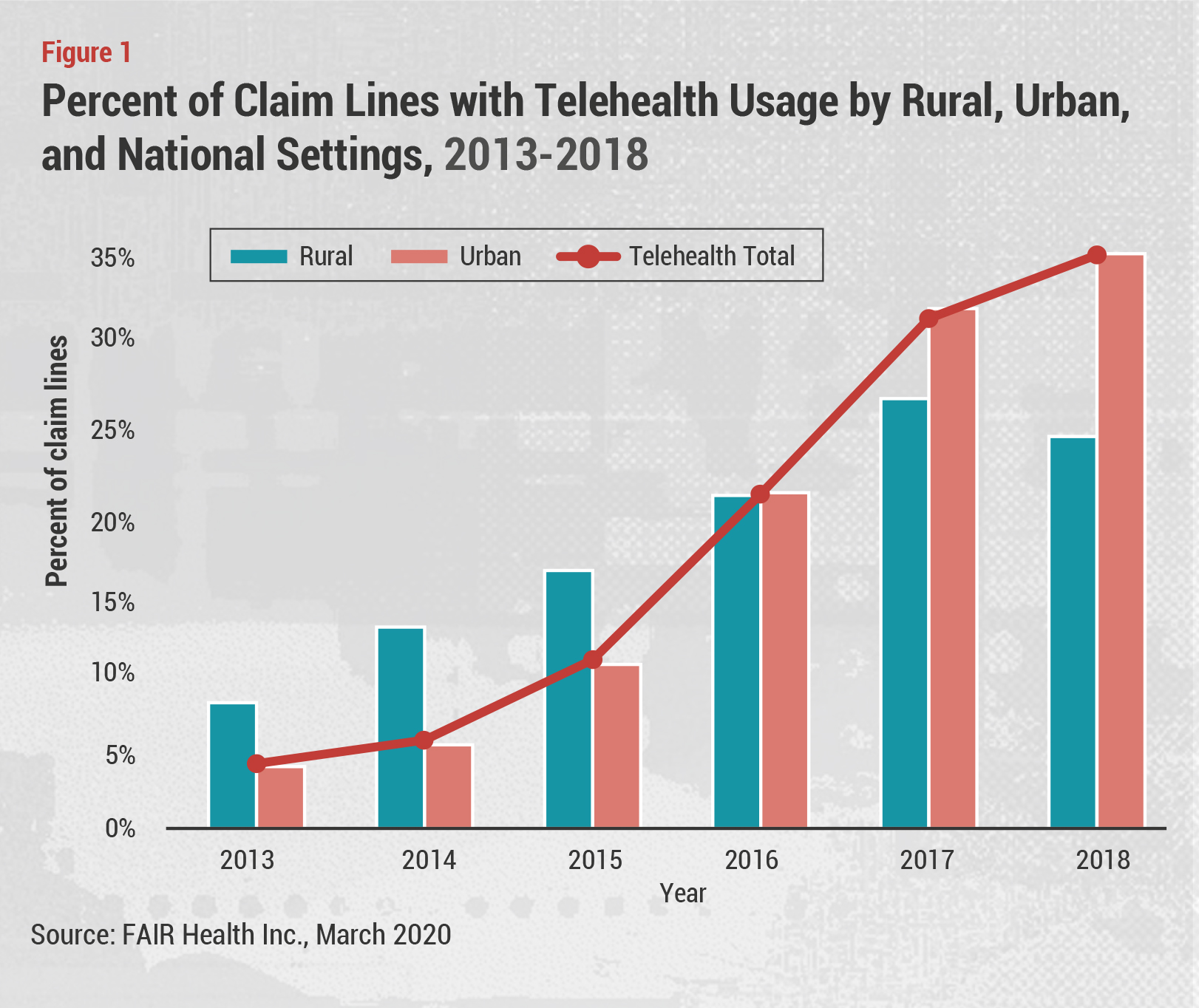 Bringing more Medicare patients on board could also positively impact physician awareness and acceptance of remote care. Although many large US hospital systems already have extensive telemedicine and remote monitoring capabilities in place, a recent survey by the AMA found that less than one-third of US physicians were using telehealth in 2019. Telehealth adoption doubled from 14% in 2016 to 28% in 2019, the survey found, but at less than 30% penetration overall, this too suggests a significant opportunity for future growth. Overall telehealth claims increased substantially between 2013 and 2018, according to FAIR Health Inc. (see Figure 1), and that trend is expected to accelerate in the coming months.
Bringing more Medicare patients on board could also positively impact physician awareness and acceptance of remote care. Although many large US hospital systems already have extensive telemedicine and remote monitoring capabilities in place, a recent survey by the AMA found that less than one-third of US physicians were using telehealth in 2019. Telehealth adoption doubled from 14% in 2016 to 28% in 2019, the survey found, but at less than 30% penetration overall, this too suggests a significant opportunity for future growth. Overall telehealth claims increased substantially between 2013 and 2018, according to FAIR Health Inc. (see Figure 1), and that trend is expected to accelerate in the coming months.
The telehealth industry is already reporting a substantial uptick in demand as a result of the COVID-19 pandemic, and with Medicare coverage restrictions now lifted, that positive momentum could carry forward well into the future. Teledoc Health, for example, which claims to be the global leader in virtual care, announced in mid-March that it was experiencing “unprecedented” daily visit volume in the US, with a 50% spike in patient visits in a one-week period and as many as 15,000 visits requested per day. The company says it provided about 100,000 virtual medical visits in the US between March 6 and 13, and it is seeing more patients with upper respiratory issues.
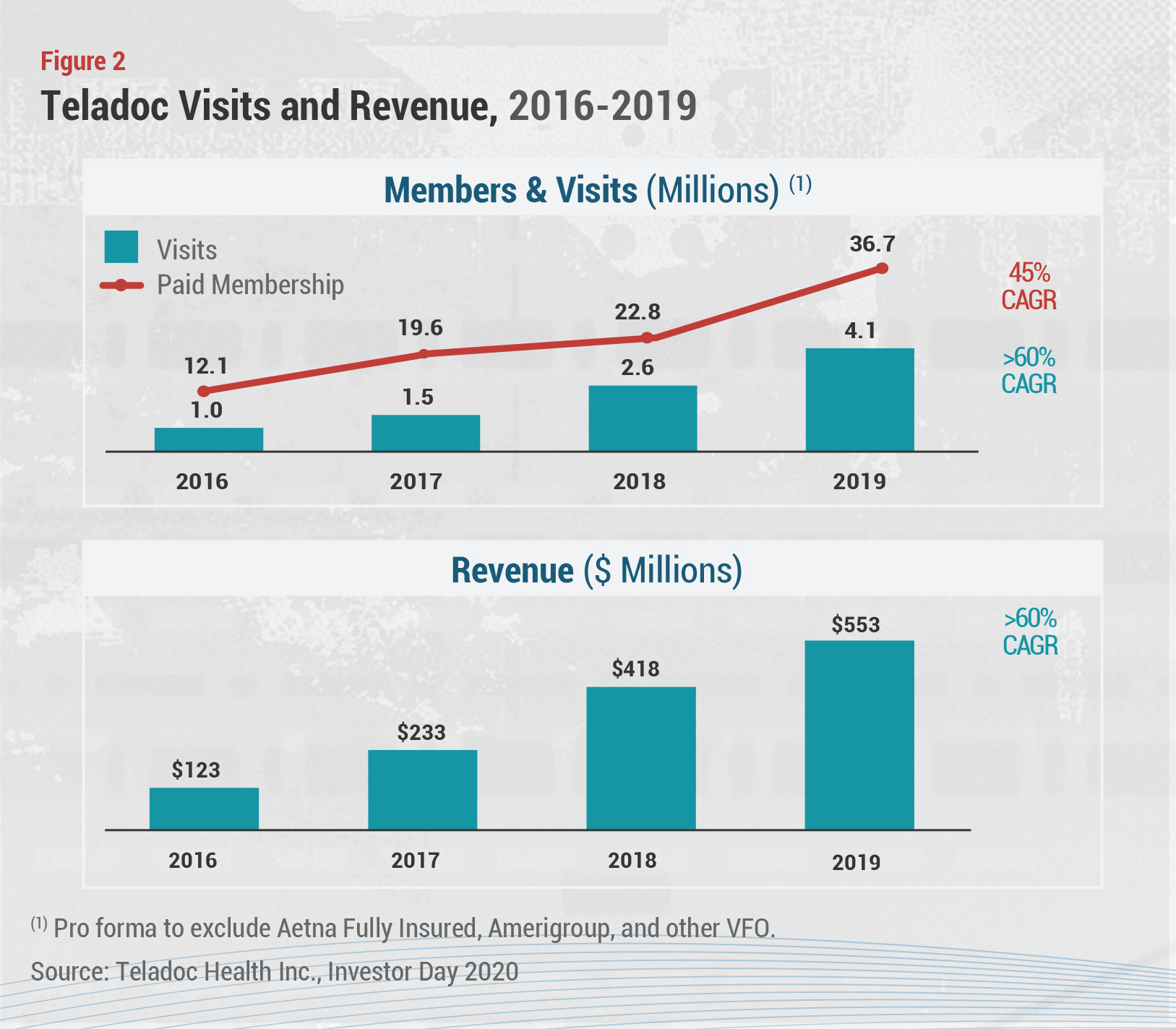 Teledoc is coming off a strong year in 2019, reporting 36.7 million US paid members as of the end of last year, a 61% increase over 2018, and more than four million visits in the year (see Figure 2.) The company hasn’t yet adjusted its 2020 guidance to account for the increases expected as a result of the COVID-19 crisis, but it has acknowledged that recent actions to ease Medicare coverage restrictions, waive consumer cost sharing, and encourage the public to take advantage of virtual care services have accelerated demand for telehealth visits, particularly among first-time users. More than half of Teladoc’s visits in the first half of March were from first-time users, the company said in a statement.
Teledoc is coming off a strong year in 2019, reporting 36.7 million US paid members as of the end of last year, a 61% increase over 2018, and more than four million visits in the year (see Figure 2.) The company hasn’t yet adjusted its 2020 guidance to account for the increases expected as a result of the COVID-19 crisis, but it has acknowledged that recent actions to ease Medicare coverage restrictions, waive consumer cost sharing, and encourage the public to take advantage of virtual care services have accelerated demand for telehealth visits, particularly among first-time users. More than half of Teladoc’s visits in the first half of March were from first-time users, the company said in a statement.
Large US hospital systems also are reporting rapid growth in demand for telehealth services. For example, the University of Pittsburgh Medical Center (UPMC), which has been on the frontlines of the movement toward digital health and telemedicine for some time now, has seen “exponential growth in video visits” in recent days, according to Graham Snyder, MD, Medical Director of Infection Prevention at UPMC, who spoke during a March 27 remote press conference held by the hospital. UPMC already had telemedicine capabilities in place but has worked over the past few weeks to increase those capabilities, he said.
In just two days during late March the UPMC hospital system performed as many telemedicine visits as it did in all of 2019.
In just two days during late March the UPMC hospital system performed as many telemedicine visits as it did in all of 2019, according to Donald Yealy, MD, Chair of Emergency Medicine at UPMC, speaking during the telepress conference. UPMC has seen a five-fold increase in demand for telehealth services, Yealy said, and the hospital system has “added or redeployed physicians and other experts, including advanced practice providers, to meet this demand.” The UPMC system now has thousands of primary care physicians and specialists who can do video visits through many different applications, he said. One area where demand is growing dramatically is urgent care, said Yealy, who noted that UPMC is now doing more urgent care visits remotely than it is doing at its urgent care centers. “Our multibillion-dollar investment in technology, infrastructure, and people in recent years made all of this possible,” Yealy said.
UPMC is also beefing up its in-hospital telemedicine capabilities, notedRachel Sackrowitz, MD, Chief Medical Officer at UPMC’s ICU Service Center. “We’ve built a 24/7 tele-ICU model where a virtual intensivist could support about 100 ICU patients, leveraging a multidisciplinary team at the bedside,” said Sackrowitz. The hospital system also has created a telemedicine-enabled infectious disease consultation company called IDConnect—a spin-off of UPMC Enterprises—with a call center that enables physician-to-physician infectious disease consultations for in-patients, not only for COVID-19, but for any infectious disease.
Other US health systems are reporting similar trends. Geisinger Health System has seen a 500% increase in telehealth visits and recently trained more than 1,000 providers to conduct telehealth visits, CIO John Kravitz recently told Paddy Padmanabhan, CEO of Damo Consulting.
Benefits and Risks
Of course, some important hurdles still exist to universal telehealth, including state-by-state differences in licensing requirements that have made it difficult for telehealth physicians to operate across state lines, uneven policies regarding payment parity, and internet bandwidth challenges in some rural areas. But many of those barriers are also beginning to fall as a result of the pandemic.
According to Kevin Harper, policy director for the American Telemedicine Association (ATA), nearly 30 states now have taken some action to allow healthcare providers in another state to be able to treat patients in their state, and that number is expected to grow. Once the crisis is over, it is hoped this will lead to a less restrictive nationwide licensing policy, or at least more cooperation among states on this issue (the Interstate Medical Licensure Compact, launched in 2017 by the Federation of State Medical Boards, enables licensed physicians to practice medicine across state lines if they meet agreed upon eligibility criteria. But so far, only 29 states and the District of Columbia have signed on to this pact. Editor's note: on April 9, CMS announced a new waiver that enables physicians to perform telemedicine visits across state lines for patients at rural hospitals.)
Notes Harper, all of this could lead to substantial growth for the telemedicine industry in the months and years ahead. But the exact impact of these recent changes, particularly the CMS waivers, is hard to predict since in many ways the industry is entering “uncharted territory.” Some 40 million Americans are currently covered by Medicare, he explains, and only a fraction has ever utilized telehealth. “That’s what I mean when I say we’re in uncharted territory. But I think we’re going to see a significant uptake over the coming months.”
Harper also believes the recent moves to free up Medicare coverage for telehealth and encourage its use could have a lasting positive impact on the remote care industry. “Congress and CMS are watching this very carefully,” he points out. “And I think they look at it as a test case for the value that telehealth can bring. My great hope is that after the crisis passes…they will [look back and] say ‘we waived all of these reimbursement restrictions for Medicare and they made a lot of sense. There’s no reason not to make them permanent.’” (See “CMS and HHS Ease Restrictions on Telemedicine During COVID-19 Pandemic,” Market Pathways, April 6, 2020.)
For example, Cleveland Clinic’s Express Care Online telemedicine service—administered by American Well—reportedly crashed multiple times in mid-March as a result of unprecedented patient demand, resulting in telehealth visit delays of more than an hour, which caused patient frustration, according to reporting by CNBC. (American Well president Roy Schoenberg, told CNBC the company has seen IT loads “quadruple,” particularly in certain geographies that have been highly impacted by COVID-19, and said the company was working to fix the issue.) Meanwhile, CNBC also reported that two other telemedicine providers, Doctor on Demand and 98point6, were frantically working to add physicians to their staff in order to meet the growing demand. Providers will need to resolve these types of issues quickly or patients (and payors) may end up with lasting negative perceptions of telehealth. That said, there is little doubt that the efforts currently being undertaken to expand telehealth and remote care will have a lasting impact on care delivery as the US moves beyond COVID-19.
Impact on Remote Patient Monitoring
As telemedicine ramps up, so will demand for digital health devices and technologies, particularly those that enable more comprehensive home-based monitoring and care for vulnerable senior populations, such as those with multiple chronic conditions. Keeping those patients at home and away from possible infection exposure is a goal that is likely to last long after the current crisis wanes. The US is already moving in that direction to a certain extent, and medtech companies that can help facilitate this shift with remote digital monitoring and therapeutics solutions could reap huge benefits in the future.
The past several years have already brought an influx of highly capable digital tools that can be integrated into a remote telehealth platform, notes Ron Emerson, RN, BSN, Global Director of Strategic Development for AMD Global Telemedicine Inc., which has seen a 500% surge in demand for its telemedicine services in recent weeks, from both new and existing customers.
Those tools include vital signs monitoring devices (temperature, blood pressure, heart rate/rhythm, oxygen saturation, etc.); imaging modalities, such as USB-enabled ultrasound devices that can remotely livestream and/or store and forward high-quality images; digital otoscopes, dermascopes, and nasal pharyngoscopes; and digital home spirometers to measure lung function. Most were originally designed to monitor patients with chronic disease, but they could also be used to assess patients for acute infectious disease, including COVID-19, and to monitor COVID-19 patients who have been discharged from the hospital. Moreover, adds Emerson, it’s not always about home-based monitoring—many of these tools can be employed in the hospital (for example, at the nurses station) to reduce clinician exposure to infected patients, or at skilled nursing facilities to improve healthcare access for this vulnerable population.
Digital RPM devices have an essential role to play in the telehealth ramp-up; in fact, telehealth and RPM go “hand-in-hand,” says Wayne Meng, Founder and CEO of PMD Healthcare, a remote patient monitoring and telehealth company. Not only can RPM deliver essential real-time biometrics data, he says, but it also can provide longitudinal trending data for individual patients, which is very important for people with chronic disease, and RPM platforms can automatically alert physicians when intervention is needed.
Founded in 2010, PMD was the first company to develop and introduce an FDA approved personal digital spirometer for home monitoring of respiratory disease patients, such as those with COPD and asthma (the company has 10 patents on the device). The company has seen a “huge surge in demand” for its RPM services in recent weeks, according to Meng, who notes that the recent changes in telehealth coverage policy have resulted in more progress in this field in the past month than has been achieved in the past several years.
Meng sees the ongoing expansion in virtual care as the “new normal” going forward. His opinion is shared widely by those in the telehealth and RPM industries, as well as by thought leaders in the healthcare community, many of whom believe the government’s groundbreaking policy shifts in favor of telehealth—and the resulting massive investments in remote workflow and infrastructure—will have far-reaching implications.
During a recent webcast hosted by telehealth company Life365, David Shulkin, MD, the former US Secretary of Veterans Affairs, characterized the current situation as a “game changer” that will have an enduring impact on the US healthcare system. “This crisis was built for telehealth,” Shulkin asserted, “and most of us believe there’s no way to put the genie back in the bottle now—we think medicine is going to be changed forever.”
Editor’s note: This article was updated post-publication.
![]() Trial MyStrategist.com and unlock 7-days of exclusive subscriber-only access to the medical device industry's most trusted strategic publications: MedTech Strategist & Market Pathways. For more information on our demographics and current readership click here.
Trial MyStrategist.com and unlock 7-days of exclusive subscriber-only access to the medical device industry's most trusted strategic publications: MedTech Strategist & Market Pathways. For more information on our demographics and current readership click here.
*End of Article*

