ARTICLE SUMMARY:
The European Parliament is expected to vote to delay the Medical Device Regulation, as the US Medicare agency rolls out multiple reimbursement policies to better support COVID-19 testing. That and much more in this week’s Pathways’ Picks.
The European Parliament is meeting for an emergency plenary session April 16-17 and the proposed one-year delay of the Medical Device Regulation is expected to come up for a vote. Meanwhile, COVID-19 reimbursement updates are flowing out rapidly in the US with a primary focus on diagnostic testing, as regulators in Europe and the US push to expand availability of new testing options. Our latest Pathways’ Picks tackles those issues and more.
EU Vote on Tap
The MDR delay is on the EU Parliament’s docket as one of a series of measures intended to address the European COVID-19 response. Final votes are anticipated for Friday. The EU Commission proposed the MDR delay earlier this month to ensure availability of medical devices in the midst of the pandemic, but it is not final until both the Parliament and the EU Council, which represents European heads of state, sign off. Look out soon for Market Pathways’ interview with MedTech Europe head Serge Bernasconi about the anticipated MDR delay.
 US Reimbursement Roundup
US Reimbursement Roundup
Also this week, the US Center for Medicare and Medicaid Services and other policymakers have been busy rolling out new policies intended make the financials work better for coronavirus testing and to help support supply of ventilators. Here are the highlights:
High-throughput reimbursement rise.Medicare says it is approximately doubling lab reimbursement for high-throughput COVID-19 testing using platforms thatcan process more than 200 specimens per day. High-throughput testing is subject to a $100 payment rate, effective April 14, compared to the $51 that Medicare Administrative Contractors will continue to pay for lower throughput assays.
No cost-sharing tests. Private insurers and employee group health plans in the US must cover COVID-19 testing with no cost-sharing when assays are used that have either been granted an FDA Emergency Use Authorization, for which the manufacturer “requested, or intends to request,” an FDA EUA, or have been authorized by a state, under guidelines issued by CMS April 11. The guidelines, which are intended to implement provisions of coronavirus relief legislation including the CARES Act, also specify that both nucleic acid and serology tests should be covered in the same manner. During the congressional process, lab stakeholders worried the policy would limit the coverage provisions to only formally FDA EUA-authorized tests, but the final guidelines provide more leeway to align with FDA’s COVID-19 emergency policies.
Serology CPTs. The American Medical Association’s CPT panel approved two new codes to support billing of COVID-19 serology (antibody) tests, for single-step and multi-step tests.
Ventilators released from competitive bidding. Non-invasive ventilators will not be included in the next round of Medicare Durable Medical Equipment Competitive bidding, CMS said April 13. That will allow any Medicare-enrolled supplier to furnish the ventilators rather than limiting suppliers to accepted bids.
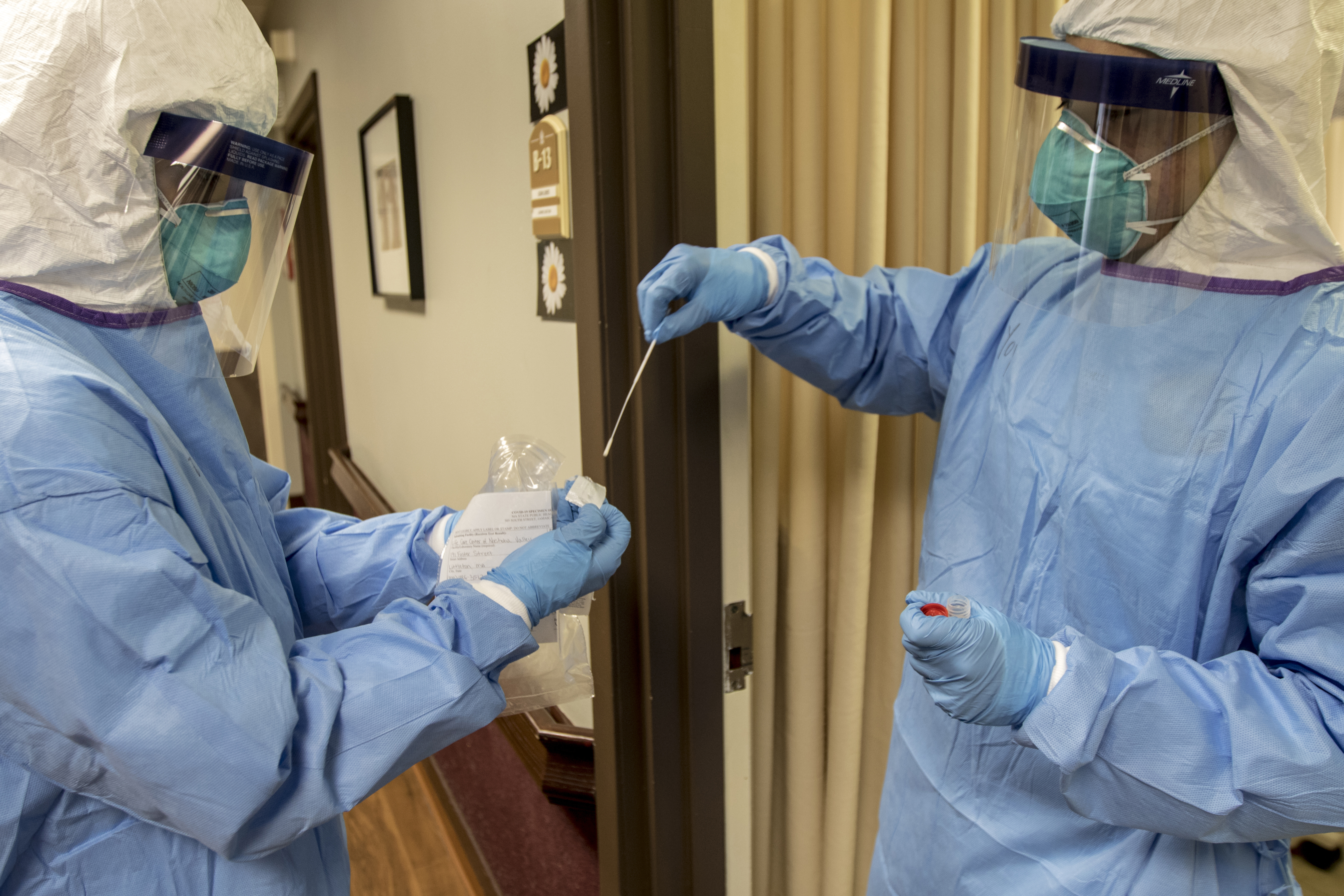 Dx Developments and Debates
Dx Developments and Debates
Building test capacity remains an intense area of focus in the fight against COVID-19. Here are some key updates from Europe and the US, and one piece of non-coronavirus diagnostics news:
EU guidelines. The European Commission issued guidelines April 15 on COVID-19 diagnostics, outlining key considerations for validating test performance. Of note, coronavirus in vitro diagnostics, as with many assays under the current IVD Directive, can be marketed based on a manufacturer’s self-certification and affixing of a CE mark without a notified body, except if the assay is intended for self-testing by the patient. The guidelines address both nucleic acid (RT-PCR) and serological antibody and antigen tests. As of early April, 78 RT-PCR tests, 13 rapid antigen tests, and 101 antibody tests had CE marks, according to the Commission.
Accuracy questions. Two Democratic members of the US House are questioning FDA on its oversight of COVID-19 test accuracy, citing recent studies in the US and UK that scrutinized the accuracy of some testing. Reps. Lloyd Doggett (D-TX) and Rosa DeLauro (D-CT) sent a letter to FDA April 9 asking for details on how the agency was collecting validation information from laboratories that have elected to start using a COVID-19 test in advance of gaining an Emergency Use Authorization under FDA’s temporary coronavirus policies. The lawmakers also say the accuracy data the agency has collected on coronavirus tests should be made publicly available. The representatives didn’t provide a specific deadline for FDA to respond to their questions.
Safety focus. In parallel, the agency has increasingly been emphasizing safety and marketing issues with COVID-19 tests. In particular, FDA diagnostics chief Timothy Stenzel said during an April 15 teleconference that FDA continues to see “problematic claims” made for some serology tests that are being offered without an EUA under a COVID-19 emergency policy (the so-called “Pathway D” policy for serology tests). FDA is also starting to circulate information on safety issues identified for certain EUA tests. Specifically, Stenzel says labeling is being updated for Abbott Laboratories Inc.’s ID NOW point-of-care SARS-CoV-2 assay to remove use of viral transport media (VTM), which reduces the sensitivity of the assay, and the agency is advising against use of certain guanidine transport media in Hologic Inc.’s Panther system because of the potential to produce toxic gas.
Blood, spit, and at-home sampling. FDA has so far held off against a strong public push for home-based COVID-19 testing, but progress is being made on that front, Stenzel said. He expects an EUA for COVID-19 testing of home-collected samples “very soon” and he says the agency is also actively working with developers of full-fledged at-home tests. This week, FDA authorized its first lab-based saliva test, developed by a Rutgers University laboratory. It also authorized two serological antibody tests this week, from ChemBio Diagnostic System Inc. and Ortho-Clinical Diagnostics Inc.
Group-based companion Dx. In non-COVID-19 news, FDA finalized a guidance outlining a regulatory framework for labeling companion diagnostics for a group of oncology drugs, rather than requiring the tests to obtain drug-by-drug approvals. Specifically, the agency is urging makers of companion diagnostics approved for testing EGFR mutations to drive therapy with individual non-small cell lung cancer drugs to submit information that will allow expanded labeling to cover all five drugs in the class.
 FDA Workarounds
FDA Workarounds
Some other notable COVID-19 medical device shortcuts granted by FDA:
Psychiatry apps. FDA is waiving 510(k) and other requirements for computerized behavioral therapy devices and other digital health therapeutic devices for psychiatric disorders including depression, obsessive compulsive disorder, insomnia, and other conditions, according to an emergency guidance document issued April 14. More tools are needed to support mental health in patients under quarantine and, generally, to support social distancing efforts.
Diaphragm pacing authorization. Synapse BioMedical Inc. was granted an Emergency Use Authorization April 13 for its TransAeris Diaphragm Pacing System to assist in weaning patients off ventilators. TransAeris is a simplified, 30-day-use version of the firm’s NeuRx DPS system, which is FDA-approved for use in patients with spinal cord injury.
Infusion pumps and nebulizers. FDA granted B. Braun Medical Inc. an EUA for several of its infusion pump systems to be used for tracheal delivery of continuous nebulized medications to COVID-19 confirmed or suspected patients. It is intended to allow treatment of critically ill patients while reducing exposure to the virus by treating clinicians.
Blood purification. FDA authorized two devices—from Terumo BCT Inc. (Spectra Optia Apheresis System) and CytoSorbents Inc. (CytoSorb)—for extracorporeal blood purification. The systems are intended to remove pro-inflammatory cytokines in certain confirmed COVID-19 patients in the ICU facing imminent respiratory failure. The goal is to reduce the risk of “cytokine storm,” a common cause of death in coronavirus patients.
More to Watch
China AE guidance. China’s National Medical Products Administration issued new guidelines earlier this month on proper procedures for conducting adverse event monitoring for medical devices in the country.
NB take on combo product. The European notified body association TEAM-NB issued a position paper on documentation requirements for drug-device combination products.
User fee meeting postponed, again. FDA had already planned a one-month delay to its kick-off meeting on the next round of device user fee negotiations. But now the agency says the meeting, which had been set as an all-virtual event for May 5, is postponed “until further notice.” FDA “continues to evaluate whether and how to proceed with upcoming scheduled meetings while our day-to-day operations are impacted by the COVID-19 public health emergency,” an April 16 notice states. The current user fee program, MDUFA IV, expires in 2022.
![]() Trial MyStrategist.com and unlock 7-days of exclusive subscriber-only access to the medical device industry's most trusted strategic publications: MedTech Strategist & Market Pathways. For more information on our demographics and current readership click here.
Trial MyStrategist.com and unlock 7-days of exclusive subscriber-only access to the medical device industry's most trusted strategic publications: MedTech Strategist & Market Pathways. For more information on our demographics and current readership click here.
*end of article*

